You’re never too young to suffer from heart disease. Many people (myself included) suffer from heart disorders, or defects, that were present at birth but only diagnosed later in life. Such heart conditions are called congenital, which means ‘present at birth’. A large portion of congenital heart disease-related deaths occur during infancy. According to the journal Circulation,
“Among infants and young children, congenital heart disease (CHD) is responsible for the largest proportion, 30% to 50%, of mortality caused by birth defects. Mortality resulting from CHD during infancy and childhood reportedly is decreasing, and the prevalence of CHD among adults is increasing.”1
Studies show that people born with congenital heart disease have a better than even chance of making it into adulthood. Whether or not those adults with congenital heart disease are likely to survive into old age is unclear. I’m sure much depends on recognizing that the problem exists and then taking action to remain as healthy as possible. But there is little doubt that the sooner heart issues are detected the better the chance for survival, regardless of age.
Tests for Congenital Heart Defects
- Fetal echocardiogram
- Echocardiogram
- Electrocardiogram
- Chest x-ray
- Pulse oximetry
- Cardiac catheterization
Fetal echocardiogram can detect various forms of heart defects in the unborn, and allows for advanced planning to improve the child’s health outcome after birth.
“Prenatal diagnosis of congenital heart disease is now well established for a wide range of cardiac anomalies. Diagnosis of congenital heart disease during fetal life not only identifies the cardiac lesion but may also lead to detection of associated abnormalities. This information allows a detailed discussion of the prognosis with parents. For continuing pregnancies, appropriate preparation can be made to optimize the postnatal outcome. Reduced morbidity and mortality, following antenatal diagnosis, has been reported for coarctation of the aorta, hypoplastic left heart syndrome, and transposition of the great arteries.”2
The fetal echocardiogram is similar to an ultrasound and is usually performed in the second trimester (18 to 24 weeks), but can be performed as early as 12 weeks into pregnancy. In the early stages, the procedure is performed through the vagina (transvaginal echocardiography), instead of the abdomen (abdominal echocardiography). Obstetricians usually recommend the procedure when previous tests detect an irregular heartbeat in the fetus. This test is considered safe and effective.
Echocardiogram is the same as the fetal echocardiogram, but for everyone else.
Electrocardiogram is a test that measures electrical activity of the heart.
“An ECG gives two major kinds of information. First, by measuring time intervals on the ECG, a doctor can determine how long the electrical wave takes to pass through the heart. Finding out how long a wave takes to travel from one part of the heart to the next shows if the electrical activity is normal or slow, fast or irregular. Second, by measuring the amount of electrical activity passing through the heart muscle, a cardiologist may be able to find out if parts of the heart are too large or are overworked.”3
This test is very safe and effective and does not send electricity into the body, as the name might imply.
Chest X-Ray is used to assess changes in the normal structure of the heart, lungs and adjacent bony structures. Heart enlargement, which can be congenital and acquired, can be evaluated with a chest x-ray. Pericardial effusion, which is a buildup of excess fluid between the heart and the membrane that surrounds it. Pericardial effusion can be seen with a chest x-ray and echocardiogram. Exposure to radiation is not without risks, but unless you are having x-rays regularly (multiple times per year) it is considered safe.
Pulse Oximetry is a test used to measure the oxygen saturation of your blood. It’s that little plastic device your doctor’s nurse sticks on the end of your finger when you have a physical. It’s an easy, inexpensive, non-invasive way to discover whether or not the heart is functioning normally. The test is administered to newborns in the UK to detect CHD and improve health outcomes for children with congenital heart disease.
Cardiac Catheterization is used to perform diagnostic tests on the heart and blood vessels, and even to treat some congenital heart conditions. It’s quite invasive, but has a low risk for complications, and can be very useful. Read ‘Cardiac Catheterization Procedures’ to learn more.
An Early Testing Success Story
I’m sure some of these tests sound unnecessary, but even the quick and easy pulse oximetry test (also known as “pulse ox”) has the power to save a child’s life.
The state of North Carolina has undoubtedly saved at least one young life with the passage of a law in 2013 that makes the pulse ox test mandatory for all newborns in the state. This simple, noninvasive test saved the life of a baby girl named Jovie Faye Smith, who was born in October of 2015. At birth, she seemed perfectly healthy. Her mother said,
“You never would have known anything was wrong with her.”4
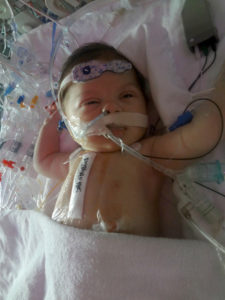
Unfortunately, there was something wrong with Jovie.
A low pulse ox reading lead to further examinations and an EKG (echocardiogram) which revealed a coarctation of the aorta – a narrowing of the major artery that carries blood from the heart to the rest of the body. To make matters worse, the left side of Jovie’s heart was mildly hypoplastic – meaning that the left ventricle was slightly underdeveloped, which affects blood flow. At 1 week old, Jovie had surgery to remove the narrow section of the aorta and the two good ends were sewn together. In addition, the doctors closed the ductus arteriosus, an opening that usually closes within two weeks after birth; Jovie’s had not closed and actually helped keep her stable prior to the discovery of her heart defect by bypassing the aorta with oxygenated blood. The operation was a success, and at 3 months old Jovie was off all medications.
It’s worth noting that the North Carolina law that saved Jovie’s life was made possible by a grassroots effort by parents and doctors, who argued that the test would save many lives by uncovering congenital heart defects at very little cost.
References
1 SM Gilboa, JL Salemi, WN Nembhard, et al. “Mortality Resulting from Congenital Heart Disease Among Children and Adults in the United States, 1999 to 2006”. Circulation, November 29, 2010. Web. February 2017
2 Simpson, John M. “Impact of Fetal Echocardiography”. Annals of Pediatic Cardiology, January-June 2009. Web. February 2017
3 “Electrocardiogram (ECG or EKG)”. American Heart Association, n.d. Web. February 2017
4 “North Carolina Pulse Ox Test Saved Jovie’s Life”. American Heart Association, n.d. Web. February 2016
Mayo Clinic Staff. “Congenital Heart Defects in Children: Test and Diagnosis.” Mayo Clinic, February 4, 2016. Web. February 2017
Mann, Denise. “EKG Testing May Spot Fatal Heart Conditions in Children”. Health Day News (Medicine Net), March 9, 2012. Web. February 2017
Kinman, Tricia. “Fetal Echocardiography: Purpose, Procedure & Risks”. Healthline, December 4, 2015. Web. February 2017
“Electrocardiogram (ECG or EKG)”. American Heart Association, n.d. Web. February 2017
“Cardiac Catheterization.” Kid’s Health, n.d. Web. February 2017